Delays in Diagnosis of Celiac Disease Worry Experts
 Clinicians are more likely to miss an early diagnosis in women with celiac disease and there is a long delay in the diagnosis of celiac disease in patients who do not present with the classic symptoms, two new studies have found.
Clinicians are more likely to miss an early diagnosis in women with celiac disease and there is a long delay in the diagnosis of celiac disease in patients who do not present with the classic symptoms, two new studies have found.
In the first study, on average, patients with celiac disease without gastrointestinal (GI) symptoms went without a diagnosis for almost four years. In the second study, the average diagnostic delay was 30% longer for women than men. Results from both studies were presented at Digestive Disease Week 2015.
Celiac disease affects approximately 1% of the population worldwide and has variable clinical manifestations. Some patients present with GI symptoms, such as bloating, diarrhea and nausea, whereas others experience weight loss, fatigue and low bone mineral density.
“Having the disease undiagnosed for a long time often leads to other long-standing medical problems, so that is why we wanted to put a spotlight on this,” said Mukund Venu, MD, assistant professor of gastroenterology at Loyola University Medical Center, in Maywood, Ill. “These medical problems include osteoporosis with potential bone fracture, an increased risk for small-bowel cancer such as lymphoma, and chronic anemia.”
Dr. Venu and his colleagues retrospectively reviewed the charts of 687 adults with a diagnostic code for celiac disease (abstract sa1302). The researchers were surprised to find that only 101 patients had undergone a biopsy, the gold standard for diagnosing celiac disease.
Among patients with biopsy-proven celiac disease, half (n=52) presented with GI symptoms and half (n=49) had unrelated complaints. The average delay in diagnosis was 2.3 months for patients with symptoms and 42 months for patients without symptoms (P<0.001). Delay was calculated as the time from first symptoms to the time of biopsy.
Patients who presented with symptoms unrelated to the GI tract were more likely to have abnormal thyroid-stimulating hormone (TSH; 43.2% vs. 15.5%; P=0.004), anemia (69.4% vs. 11.5%; P<0.001) and low bone density (68% vs. 41%; P=NS).
“It is important for providers, primary care doctors as well as GI doctors to be aware of the global picture of celiac disease,” Dr. Venu said. “Just because someone doesn’t have GI symptoms doesn’t mean they don’t have celiac disease. It is an important diagnosis to keep in your differential when you are evaluating patients.”
In a second study, researchers reviewed the records of 1,689 patients diagnosed with celiac disease in Switzerland since 1970 (abstract sa1275). Roughly three-fourths were female; the average age was 41.3 years; and the average age at diagnosis was 31 years. The researchers focused on evaluating diagnostic delay, which can be subdivided into patient delay, defined as the gap between the beginning of symptoms and first medical consultation, and doctor delay, defined as the gap between first medical consultation and a definitive diagnosis. The average total diagnostic delay was 87 months, with the delay split equally between patients (40.8 months) and physicians (37.9 months). The median delay was 24 months.
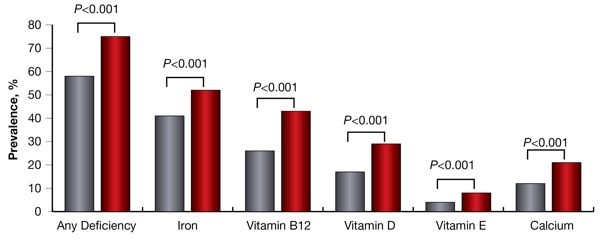
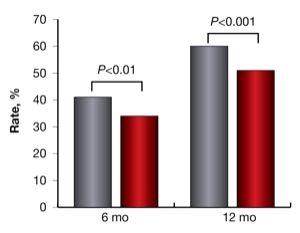
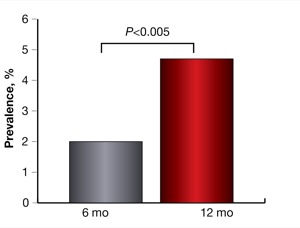
Longer diagnostic delay was associated with a more frequent need for immunosuppressants to treat celiac disease, more frequent nutritional deficiencies and a lower chance of clinical remission after diagnosis (Figure 1). An increased diagnostic delay of more than two years was associated with a lower chance of clinical remission six and 12 months after diagnosis (Figures 2a and 2b).
|
||||||||||||||||
Women had longer diagnostic delays than men, and this difference was attributable solely to the physician (Table). The researchers also found that patients who were older than 30 years were more likely to have longer diagnostic delays than patients younger than 30.
A total of 15.3% of patients reported that irritable bowel syndrome (IBS) was diagnosed or suspected by their treating physicians before establishing the diagnosis of celiac disease, with more women than men reporting this experience (16.7% vs. 10.5%; P=0.004).
Stephan Vavricka, MD, of the Division of Gastroenterology and Hepatology at Triemli Hospital, in Zurich, who led the study, said physicians “need to think earlier about celiac disease, especially in women, where you expect IBS.”
Christina Tennyson, MD, a celiac specialist and physician in the Department of Gastroenterology at Icahn School of Medicine at Mount Sinai, in New York City, said the studies add to the growing evidence that many patients who present with celiac disease do not have classic GI symptoms (Am J Med 2006;119:355.e9-e14).
The recent availability of screening blood tests for the condition, such as tissue transglutaminase antibody IgA, has helped in diagnosis, but there is a need for more education of doctors and patients about the prevalence and symptoms of celiac disease, she said.
“The majority of patients who have celiac disease aren’t diagnosed,” said Dr. Tennyson, who was not involved in the latest research. “We need to increase physician education and awareness that celiac disease can present many different ways.”
According to Dr. Tennyson, the Swiss study was particularly interesting because it found that “although greater numbers of women are diagnosed with celiac, they are more likely to have a delay in their diagnosis.” The study also has an important clinical message, she added: “If you diagnose the patient quicker, this suggests that there is an improved clinical course.”
Excerpted from https://www.gastroendonews.com/ViewArticle.aspx?d=In+the+News&d_id=187&i=July+2015&i_id=1207&a_id=32940 by Kate O’Rourke