Father Shares Son’s Celiac Disease Diagnosis
Remember when it happened to us? While we know how easy – and how important it is – to be gluten free, this father’s story reminds us of how hard it continues to be for children suffering from a host of symptoms to achieve a diagnosis. William Kremer shares his son’s journey to diagnosis

In February, my 21-month-old son Sam went down with what appeared to be a nasty virus. My wife and I set about dealing with the vomiting and diarrhoea, expecting things to improve in a few days.
But as the weeks passed, we began to wonder what kind of virus this could be. Normally a force to be reckoned with at the table, Sam began to pick at his food and lose weight. At bath time we could see the outline of his ribs above his belly, which had swollen up like a balloon.
He stopped walking or even being able to stand, and his sunny personality shaded over. He screamed at strangers and refused to make eye contact or even look in a mirror. Day and night, the house was filled with the sound of jarringly upbeat nursery rhymes playing on a loop from YouTube – watching them was the only thing that seemed to bring him any pleasure at all.
One day, feeling overwhelmed, we went to the hospital emergency department, and it was there that a paediatrician first mentioned an illness that I had never heard of before. I had no idea what coeliac disease was, or even how it was spelled. A blood test and biopsy confirmed that my son had this autoimmune condition that is fed by gluten, a protein. Gluten is found in wheat, and very similar proteins are present in barley and rye. Even a crumb of bread, we were told, was enough to send Sam’s body haywire. Sam, looking anaemic, the day before we removed gluten from his diet. We took him for a final gluten blowout, but he only touched his water.
Sam – and I mean this in the nicest possible way – is an evolutionary throwback. Go back more than 10,000 years and everyone was on a gluten-free diet. Then they started farming – an agrarian revolution that gave our species the free time to build civilisations and develop culture and technology.
Human beings generally have a lot to thank gluten for. It makes our bread light and springy, since it is able to trap steam and carbon dioxide as dough rises, and during baking.
But it is unique among proteins in that it cannot be broken down completely by human beings into amino acids. The best we can manage is to break it into chains of acids called peptides. These simply pass through most people’s bodies, but coeliacs are genetically predisposed to flag them up to the immune system, which believes it is being attacked by microbes.
A war begins, and there is collateral damage: a flattening of the villi, the finger-like fronds that line the small intestine and absorb nutrients into the bloodstream. As they become stunted, their surface area decreases and they cannot do their job properly. When the gastroenterologist showed me pictures of Sam’s small intestine it was red and inflamed. (I didn’t really know what I was looking at, but he assured me it wasn’t good.)
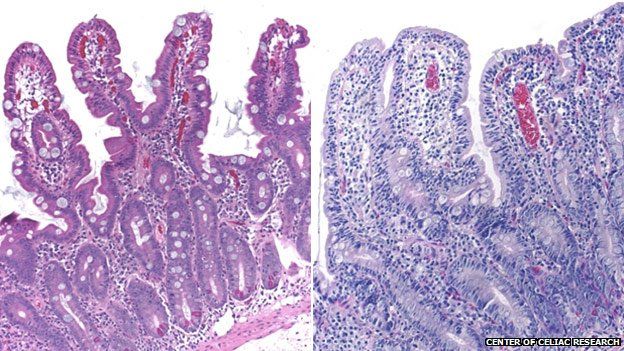
There are many alarming long-term effects of untreated coeliac disease, ranging from stunted growth to bad skin rashes and – in rare cases – intestinal lymphoma. Worryingly, most people who have it don’t know about it and may not even have any obvious symptoms (in the UK only 24% of sufferers are diagnosed). It’s unknown why it “switches on” at any given time and there is currently no cure, but there is a simple treatment – steer clear of gluten.
About a week after we started to do this, Sam began to brighten up and put on weight. He gained two kilos in two weeks – the amount children his age typically put on in a year. Before too long, the little boy we had not seen for some months came back.
Coeliac disease is quite common, afflicting about 1% of people in the developed world, but it isn’t enough to explain the burgeoning popularity of the gluten-free diet. According to Mintel, 7% of UK adults say they avoid gluten because of an “allergy” or “intolerance” (strictly speaking, coeliac disease is neither of those), and a further 8% avoid it as part of a general “healthy lifestyle”.
This view, that gluten isn’t just bad for coeliacs like Sam, but for everyone, is endorsed by bloggers, best-selling nutritionists and celebrities. A report on the US gluten-free market by Mintel values it at almost $9bn, because “the health halo surrounding the gluten-free category continues to drive general consumer interest”. The singer Miley Cyrus encapsulated the mood in a tweet: “Gluten is crapppp anyway!”
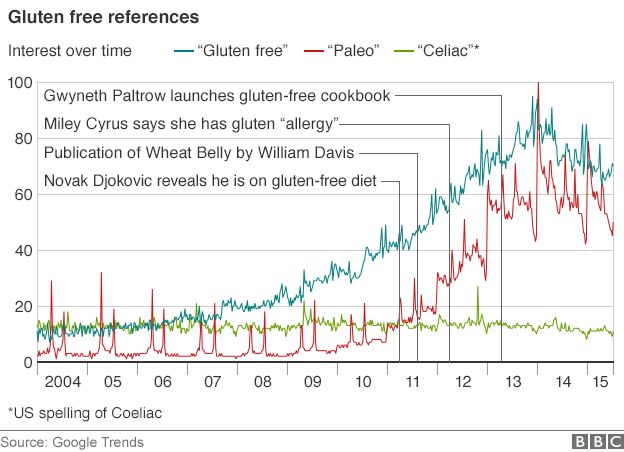
A glance at internet searches over the years suggests that the rise of interest in gluten-free diets has little to do with a growing awareness of coeliac disease, and a lot to do with the popularity of “paleo” diets – the food movement that seeks to return humankind to the Stone Age, at least as far as diet is concerned.
I did my own journalistic hunter-gathering at the Allergy and Free From exhibition in west London, a beacon for all loathers and avoiders of gluten, dairy, nuts and the like. The exhibition was actually a three-in-one, as this year a vegetarian / vegan show and an organic show were bolted on to the allergy exhibition.
“When we were starting to ask the [allergy] audience about other things they were interested in, it turns out we had 40% or 50% vegetarians or vegans coming through the door,” Tom Treverton, the event’s director, told me. While some of the show’s 35,000 visitors would just be looking for niche products to answer their particular dietary need, “there is an emerging trend in the Free From lifestyler – that is the person who wants to cut something out of their diet for another reason – not because they’re allergic to it, but because they feel better when they do it, and they think it might be healthier.”
The crossover isn’t just with organic and vegetarian food. You don’t have to wander far past the cakes, beers and salty snacks to find yourself looking at acupressure mats and energy balls. A surprising number of pet charities were also present at the event.
“I didn’t think I’d like it, but it’s brilliant, so I’d definitely consider it,” one woman told me, speaking about the gluten-free diet that my son must follow for the rest of his life. Most people I spoke to, though, had genuine health concerns. I met coeliacs on a mission to find a decent loaf of bread or bottle of beer, but I spoke to even more people who described themselves as “gluten intolerant”.
“It’s terribly embarrassing to turn up at a social event with swollen lips or a swollen face,” said Elizabeth Jones, referring to an intolerance she began suffering from 15 years ago. Gluten was just one of a number of foods that she cut from her diet – the list also included grapes – which, by trial and error, seemed to alleviate her symptoms.
Another woman, Debra from Hertfordshire, used to suffer from acid reflux. She was checked for coeliac disease, and found not to have it, but a hospital dietician nevertheless recommended that she cut gluten from her diet. It seemed to do the trick. Debra herself is a paediatric gastroenterology nurse. She told me she saw a large number of children, whose villi were undamaged and therefore got a negative biopsy result – but like her, their condition improved when they stopped eating gluten.
What’s wrong if indeed someone feels better going gluten-free, not because gluten harms them, but because they feel they are doing something that’s going to benefit them?
 In February 2011, some of the world’s leading researchers on coeliac disease met in a hotel near Heathrow Airport in London to discuss patients like Debra, who had many of the outward signs of coeliac disease but few of the inward ones. A report of this meeting, published in the journal BMC Medicine, proposed that doctors broaden their scope from just looking at coeliac disease, to a “spectrum of gluten-related” disorders, with coeliac and wheat allergy (which affects a tiny minority of people) at one end of the spectrum, and “non-coeliac gluten sensitivity” at the other
In February 2011, some of the world’s leading researchers on coeliac disease met in a hotel near Heathrow Airport in London to discuss patients like Debra, who had many of the outward signs of coeliac disease but few of the inward ones. A report of this meeting, published in the journal BMC Medicine, proposed that doctors broaden their scope from just looking at coeliac disease, to a “spectrum of gluten-related” disorders, with coeliac and wheat allergy (which affects a tiny minority of people) at one end of the spectrum, and “non-coeliac gluten sensitivity” at the other
The existence of gluten sensitivity remains disputed, but one of the men in the room in 2011, Dr Alessio Fasano, director for the Center of Celiac Research in the US, is a believer. His open-minded attitude is a result of his remarkable experience treating coeliac disease in North America.
In 1993, he took up the post of director of paediatric gastroenterology at the University of the Maryland School of Medicine. He was a young doctor from Naples in Italy, where he had seen perhaps 20 or 30 children a week with coeliac disease.
It was a different story in the US. “The days, the weeks, the months passed by – and I did not see a single case of coeliac. Not a single case,” he recalls. In 1996, Fasano published a paper in a paediatrics journal entitled Where have all the American coeliacs gone? The research, based on analysis of 2,000 blood samples that Fasano bought from the Red Cross, contended that there were just as many coeliacs in the US as there were in Europe, but because the disease was so narrowly defined in America, they were being misdiagnosed.The reception from his peers was sceptical. So Fasano and his team launched a much larger epidemiological study of 13,000 people. This helped shift the estimated prevalence from one in 10,000 to one in 133. His clinic now treats more than 1,000 patients a year.
Unlike wheat allergy and coeliac disease, gluten sensitivity does not have a known set of biomarkers – doctors can’t tell if a patient is suffering from it by examination (although there is a blood test, it doesn’t give accurate results for many patients). So it can only be diagnosed by first ruling out other diseases and then trying out a gluten-free diet.
Although gluten has no nutritional value in itself, making a radical change to one’s diet without the supervision of a dietician is a bad idea, Fasano insists. “Going gluten-free deprives you of many key elements of the diet, like vitamins and fibres that need to be supplemented in order to maintain balanced nutrition,” he says.













